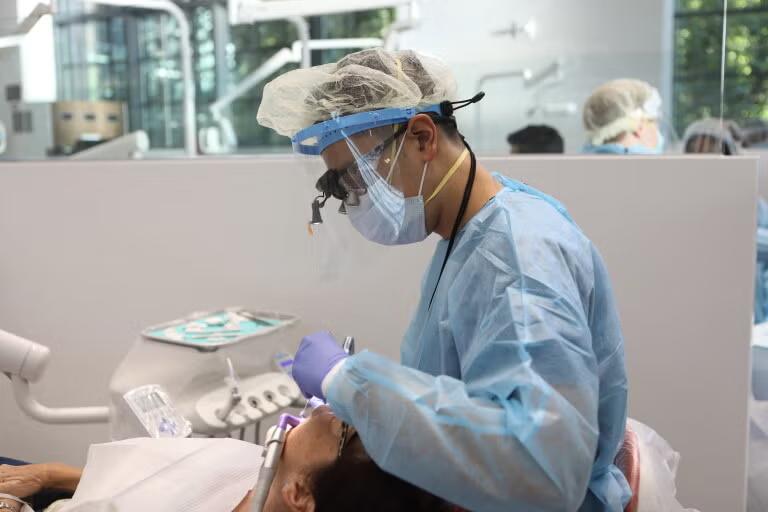
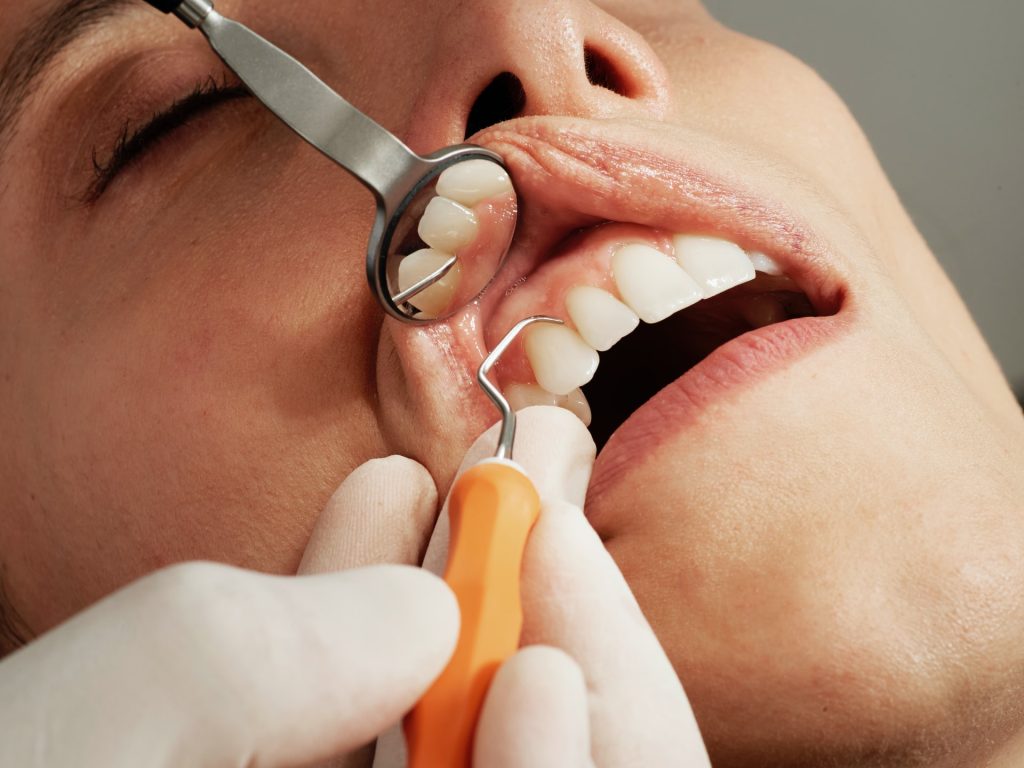
People living with HIV now have a longer life expectancy and commonly seek dental care. HIV infection is not a contraindication for dental treatment. With standard infection control and ethical practice, dentists can safely manage these patients.
Patient Rights and Ethics
- Maintain strict confidentiality of HIV status
- Never disclose medical information without patient consent
- Discrimination based on HIV status is unethical and unacceptable
Infection Control in Dental Practice
Clinic Preparation
- Clean and disinfect all instruments and surfaces
- Use sterile instruments and disposable items
- Line waste bins with plastic bags
- Dental staff must wear gloves, masks, gowns, and eye protection
During and Between Patients
- Do not refill local anesthetic syringes
- Use over-gloves or an assistant for touching common surfaces
- Disinfect trays and spittoons after each patient
- Change handpieces, ultrasonic tips, curing tips, tumbler, and bib
- Dispose disposables safely and sterilize reusable instruments
End-of-Day Protocol
- Clean trays, spittoons, floors, and walls
- Remove waste bags for proper disposal
- Flush air-rotor and water lines for 2–3 minutes
Personal Protection for Dental Staff
- Wash hands before and after each patient
- Use antiseptic handwash (e.g., chlorhexidine)
- Change masks between patients or hourly
- Check gloves for damage and discard if defective
- Clean protective eyewear after use
Instrument & Surface Management
- Clean, dry, lubricate, and autoclave instruments
- Heat sterilize handpieces and burs
- Disinfect or barrier-cover non-sterilizable surfaces
- High-touch areas must be disinfected after every patient
Aerosol Control
- Pre-procedural mouth rinse is advised
- Procedures are to be done under Rubber dam isolation
- High-volume suction and saliva ejectors are recommended
Medical Assessment Before Treatment
- Review current medications, including antiretroviral therapy.
- Check history of opportunistic infections.
- Assess bleeding risk and review relevant blood tests (CBC, platelet count, CD4 if available).
- Note low platelet (<60,000/mL) or neutrophil (<500/mL) counts.
- Evaluate potential drug interactions with antiretroviral therapy.
- Use antibiotics only when clinically necessary.
Dental Care for HIV-Positive Patients
Initial Assessment
- Complete oral examination: soft tissue, gums, and teeth.
- Identify any HIV-related oral manifestations.
Regular Monitoring
- Continuous follow-up to track disease progression.
- Focus on relieving pain and treating infections.
Prevention and Counseling
- Guide on proper oral hygiene.
- Advise on avoiding risk factors: tobacco, alcohol, or drugs.
Routine Dental Care
- Most HIV patients tolerate standard procedures, including oral surgery.
- Individualized treatment planning in consultation with the patient and physician.
Surgical Procedures
- Same indications as for other patients.
- Preoperative scaling to reduce complications.
- Minimize bleeding and avoid spreading infection into deeper tissues.
Dental Treatment Guidelines
- Treat HIV patients similar to non-HIV patients
- No routine antibiotic prophylaxis based solely on HIV status
- Treatment depends on overall medical condition
- Preventive care and oral hygiene maintenance are essential
Pain, Anxiety & Drug Considerations
- Local anesthetics are safe
- Nitrous oxide and short-acting anxiolytics may be used
- Prescribe analgesics carefully due to drug interactions
Post-Exposure Management
- Wash injuries with soap and water
- Flush eyes or mouth with clean water
- Report immediately and seek medical care
- Antiretroviral medications can be used as post-exposure prophylaxis (PEP) if started within 72 hours of potential HIV exposure. Early initiation significantly improves effectiveness. A commonly used PEP regimen includes Zidovudine combined with Lamivudine, taken for a 4-week course to reduce the risk of infection.
HIV infection is not a reason to deny dental treatment. By following universal precautions, ethical principles, and proper clinical protocols, dentists can safely deliver effective, compassionate, and high-quality oral care to patients living with HIV.
References
- ADA – Human Immunodeficiency Virus (HIV) and Dental Care
A comprehensive overview of infection control and routine dental management for HIV patients.
https://www.ada.org/resources/ada-library/oral-health-topics/hiv (American Dental Association) - CDC – Guidelines for Infection Control in Dental Health-Care Settings
Standard infection control recommendations to prevent pathogen transmission in dental practice.
https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm (CDC) - CDC – Oral Health Care for People Living With HIV/AIDS (Dental Case Manager Approach)
Discusses dental care challenges and strategies for oral health in HIV/AIDS populations.
https://www.cdc.gov/pcd/issues/2012/11_0297.htm (CDC) - IDA – Treating Patients with HIV (Indian Dental Association)
Ethical obligations and practical infection control guidance for dentists treating patients with HIV.
https://www.ida.org.in/Membership/Details/TreatingPatientswithHIV (Indian Dental Association)