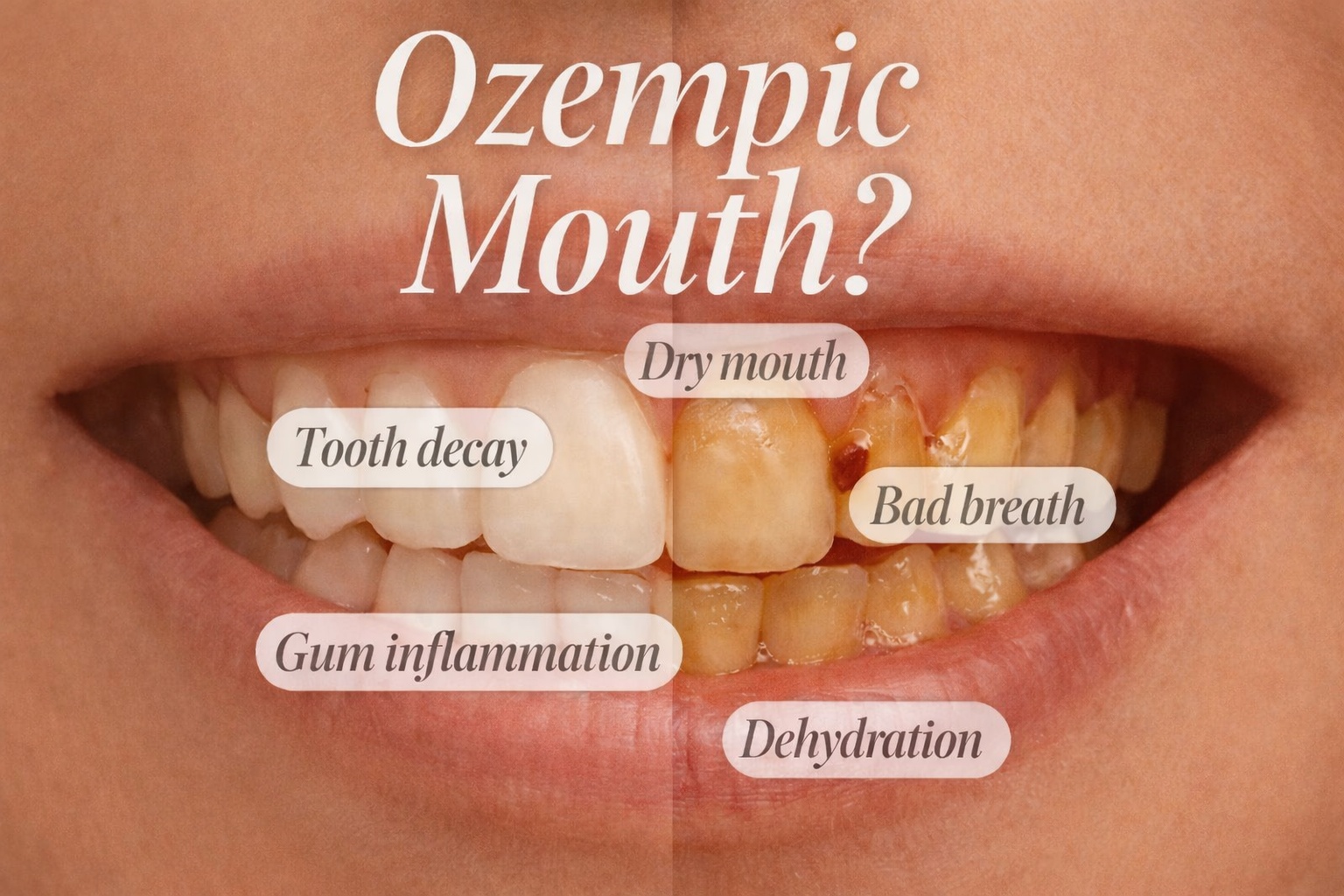
Injectable weight-loss and diabetes medications such as semaglutide and tirzepatide are transforming metabolic care worldwide. However, dental professionals are now reporting a noticeable rise in oral health complaints among patients using these therapies – an emerging concern gaining attention in clinical practice.
Though often referred to informally as “Ozempic-related dental problems,” this is not a defined medical condition. Instead, it describes a pattern of rapid tooth deterioration, enamel weakening, gum irritation, and oral discomfort seen in some individuals undergoing GLP-1–based treatment.
Why are teeth affected?
The medications do not attack teeth directly. Instead, their systemic effects create an oral environment that increases vulnerability.
Reduced saliva production
Many users experience persistent dryness of the mouth. Saliva is essential for buffering acids and controlling harmful bacteria. When salivary flow decreases, decay can progress quickly and silently.
Acid exposure from gastrointestinal side effects
Episodes of nausea or reflux can repeatedly bathe teeth in stomach acid, leading to surface erosion, translucency, and sensitivity, especially on enamel already under stress.
Nutritional compromise
Strong appetite suppression may result in inadequate intake of micronutrients necessary for oral tissue health, weakening the gums and slowing natural repair mechanisms.
Interrupted oral hygiene habits
Fatigue, nausea, or general discomfort may cause patients to unintentionally neglect brushing and interdental cleaning, accelerating plaque accumulation.
What dentists should watch for
Practicing dentists may notice:
- Sudden increase in caries activity
- Cervical and palatal enamel erosion
- Inflamed or bleeding gingiva
- Unexpected tooth mobility in non-periodontitis patients
Early recognition allows intervention before irreversible damage occurs.
Preventive strategies for patients
Dental teams should emphasize simple but effective protective measures:
- Encourage frequent water intake to combat dryness
- Recommend saliva substitutes or stimulants
- Advise rinsing with water after vomiting — delay brushing
- Stress the importance of continued nutrition despite reduced appetite
- Reinforce consistent oral hygiene routines
Lifestyle triggers such as alcohol, tobacco, caffeine, and acidic foods should be minimized.
Interdisciplinary care matters
When dental symptoms coincide with ongoing GLP-1 therapy, communication between dentists, physicians, and patients becomes essential. Adjusting medication dosage or managing gastrointestinal effects may significantly reduce oral complications.
The broader message
Modern medications can dramatically improve metabolic health, but oral health should not become collateral damage. As this trend becomes more visible, dentists play a critical role in early detection, education, and prevention.
Healthy weight loss should never come at the cost of healthy teeth.
REFERANCE
- Healthline — Ozempic Teeth and Dental Side Effects
“‘Ozempic Teeth’ May Cause Tooth Decay, Other Dental Health Effects” — covers dry mouth, enamel erosion, and why these issues are being reported among GLP-1 users. Healthline: Ozempic Teeth Dental Side Effects Explained - American Dental Association (ADA) Coverage of Oral Effects
- “Ozempic may yield weight loss but also bad breath” — discusses dry mouth and oral health complaints tied to GLP-1 drugs like Ozempic. ADA News on Ozempic and Oral Health Risks